| CLICK HERE and let us discuss how BHM’s clients benefit from our in-depth data-based reporting, analysis, and consultations. |
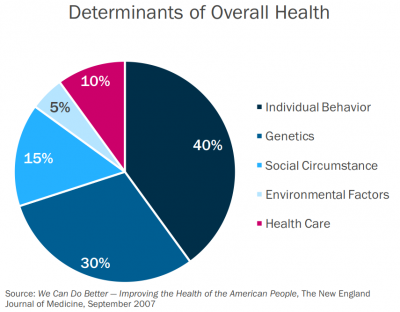 Currently, payer strategies focus on finding healthy populations, segmenting the markets, and segmenting populations, with the target of avoiding costly procedures. Population management and all the big data trends became useful tools in those payer strategies. With the results from a study by the Robert Wood Johnson Foundation and a position paper by America’s Health Insurance Plans (AHIP), social determinants quickly rose as the next measurable data used by payers.
Currently, payer strategies focus on finding healthy populations, segmenting the markets, and segmenting populations, with the target of avoiding costly procedures. Population management and all the big data trends became useful tools in those payer strategies. With the results from a study by the Robert Wood Johnson Foundation and a position paper by America’s Health Insurance Plans (AHIP), social determinants quickly rose as the next measurable data used by payers.
“Plans have moved beyond traditional medical care to provide coordinated social services and educational opportunities to plan members while connecting them with community-based organizations,” from AHIP report. The report continues with nine cases of payers turning social determinant data into successful programs.
Payers Using Social Determinants
Download the report for details on the programs from, Anthem, CareSource, Harvard Pilgrim Health Care, Health Net, Humana, Kaiser Permanente, L.A. Care Health Plan, Molina Healthcare, and UPMC Health Plan. According to a report from AHIP, these determinants have an extremely potent effect on an individual’s overall health.
CareSource Life Services JobConnect, a pilot program in Ohio and statewide in Indiana and Georgia (July 2017), is designed to help members get and keep jobs that can improve their lives. The program identifies and addresses gaps in members’ educational needs, interview skills, employment assistance, and job training. CareSource then links members with employer partners to improve long-term financial stability through employment.
“Billions in overspending on medical costs are attributed to social determinants of health (SDOH), and SDOH can identify if beneficiaries covered by insurance plans are at risk for adverse health conditions outside their coverage,” writes Thomas Beaton for HealthPayerIntelligence.com.
“Healthcare organizations today are expanding their ideas of what influences a patient’s health beyond orange pill bottles and family history,” writes Kate Monica for her article, Evidence Supports Push for Social Determinants in EHR Data. “Research and use cases are providing support for the push to integrate social determinants of health data into EHR data.”
Elizabeth H. Bradley and Lauren A. Taylor, two authors of the Robert Wood Johnson Foundation study, Variation In Health Outcomes: The Role Of Spending On Social Services, Public Health, And Health Care, 2000–09, reported social determinants of health have been linked to better patient outcomes and reduced medical expenditures.
“Our study found this same pattern within the United States:
- When comparing state-to-state spending between 2000 and 2009, those states with higher ratios of social service spending to health care spending had better outcomes on average. The size of the health effects were substantial. For instance, a 20 percent change in the median social-to-health spending ratio was equivalent to 85,000 fewer adults with obesity and more than 950,000 adults with mental illness.
- Many of the states with higher ratios of social to health care spending were in the West, while those with less healthy spending patterns were in the South; states in the Midwest and Northeast had more mixed profiles.
- We examined health outcomes for adult obesity, asthma, mentally unhealthy days, days of activity limitations and mortality rates from lung cancer, acute myocardial infarction and type 2 diabetes. Our findings suggests that the allocation of spending, not just the total investment, may be key to improving health outcomes.”
CLICK HERE and let us discuss how BHM’s clients benefit from our in-depth data-based reporting, analysis, and consultations.