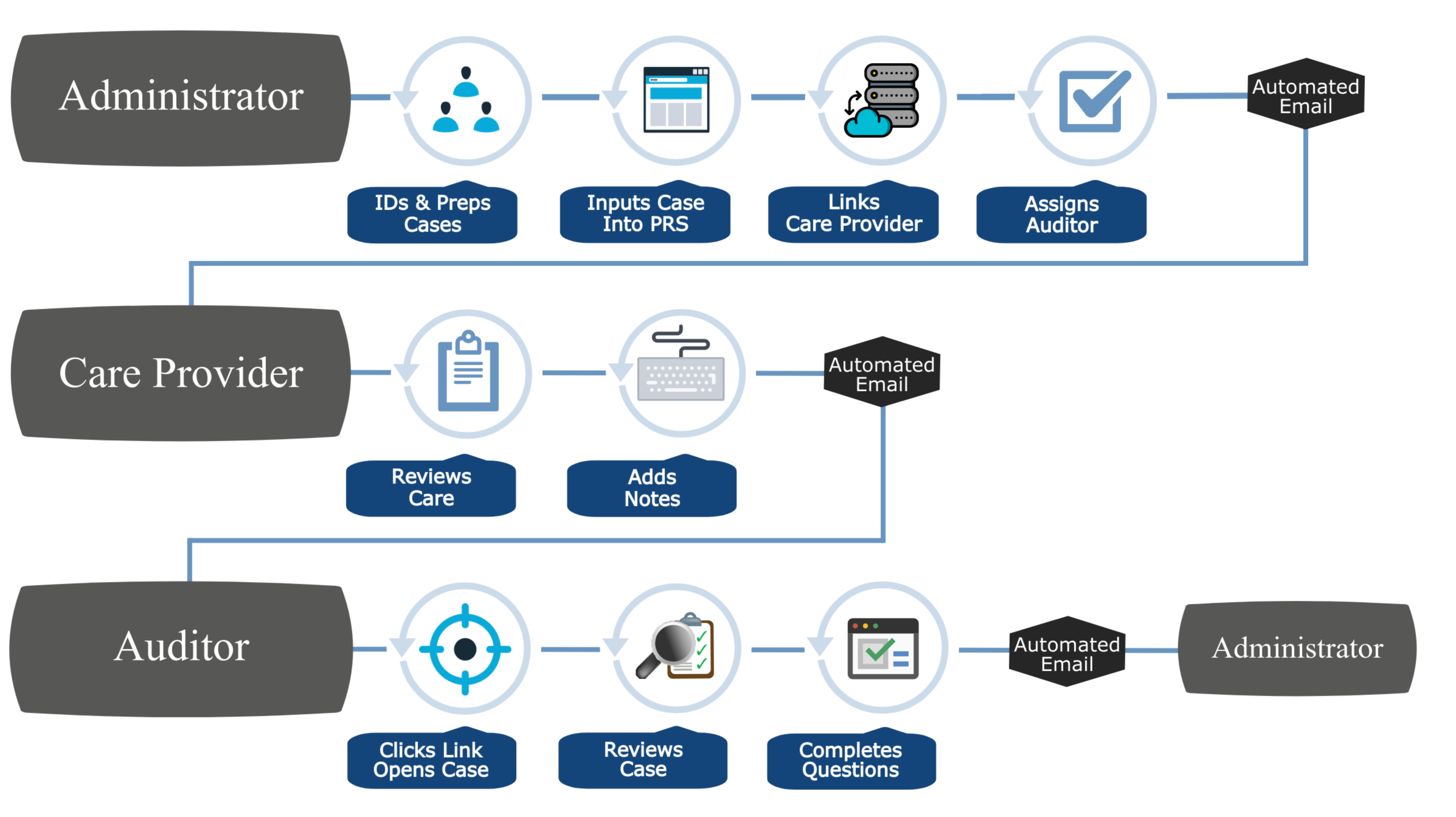
Medicaid Growth in 2022/23 and the Impact on Underserved Populations
Medicaid growth has been driven by several factors, including changes in federal policy, public pressure, and a greater understanding of the benefits of Medicaid for underserved populations.