Summary: How does an organization rise to the challenge of transitioning from volume to value and from quantity to quality?
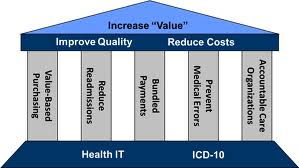 The transitioning from volume to value and from quality to quality is at the moment a bit of a juggling act. Medicare continues to reimburse based on a fee-for-service basis which rewards based upon volume and quantity while simultaneously moving toward a payment system based upon value and quality. Two completely opposite ends of the spectrum trying to exist concurrently. Two different philosophies and mindsets with different goals are colliding.
The transitioning from volume to value and from quality to quality is at the moment a bit of a juggling act. Medicare continues to reimburse based on a fee-for-service basis which rewards based upon volume and quantity while simultaneously moving toward a payment system based upon value and quality. Two completely opposite ends of the spectrum trying to exist concurrently. Two different philosophies and mindsets with different goals are colliding.
One of the predominant issues with healthcare is increased costs. Costs are skyrocketing out of control. Additionally, emphasis is shifting toward quality patient care. Unfortunately with the current fee-for-service delivery system, there is no correlation between costs and quality. Costs continue to rise while quality is remaining the same or even decreasing. Coordination of care is almost non-existent. Inefficiencies within the healthcare system are of vital concern.
So, how does an organization/practice begin transitioning from volume to value and from quantity to quality?
The keyword is transition. Transition infers a process over time, not an over-night venture. There are many things an organization can begin focusing upon to ensure a smoother transition:
- Begin reviewing processes and procedures. Map out each step and begin to look for inefficiencies and waste. Begin determining who in the organization, both physicians and staff, will be most appropriate to take ownership of these processes and to begin making changes. A tweak here and there can go a long ways towards attaining efficiency.
- Begin looking at new pay models which can help bridge the gap between volume and value. Some of these methods include bundled
 payments, patient centered medical homes and accountable care organizations. These pay models are designed to reimburse based upon quality, collaboration, and accountability. The CMS website has many innovations and programs which are in the works with detailed information as to how to take advantage of them.
payments, patient centered medical homes and accountable care organizations. These pay models are designed to reimburse based upon quality, collaboration, and accountability. The CMS website has many innovations and programs which are in the works with detailed information as to how to take advantage of them. - Primary care is the key to care coordination. According to the Affordable Care Act, primary care can assist in bridging the gap between quantity and quality. In this model, primary care providers are responsible for coordinating care between specialists, labs, diagnostic imaging centers, rehab facilities, hospitals, etc. Additionally, the patient is placed at the center of their care and involved in decisions affecting their healthcare outcomes. Primary care is the key to reducing unnecessary readmissions. Upon leaving the hospital, primary care becomes involved to ensure the patient transition home or to another facility is smooth. Follow-up is important to ensure the patient has appropriate appointments scheduled, that they actually show up for those appointments, that their medications are being taken appropriately, and any changes in medical condition following discharge are immediately addressed.
- Begin moving towards healthcare analytics for clinical, operational, and financial perspectives. Data is a key element in progressing toward a value driven society. Metrics need to be developed, implemented, tracked, and revised on a constant basis. Even more important is beginning to develop the infrastructure needed to physically house the data. This is especially true with Health IT and Electronic Health Records systems. Allowing more access to protected information requires additional security measures to be taken. Health IT and the infrastructure thereof can be very costly investments. Beginning the process early allows the costs to be spread out over a greater period of time.
 Begin focusing on the well-being of your staff with employee health programs. Some of the waste attributed to the healthcare system is through employees. Countless dollars are lost as well as reduced productivity through not focusing upon employees through both prevention as well as safety issues/workers’ compensation. Wellness programs and rewarding for engaging in healthy activities can shave quite a bit off of healthcare spending.
Begin focusing on the well-being of your staff with employee health programs. Some of the waste attributed to the healthcare system is through employees. Countless dollars are lost as well as reduced productivity through not focusing upon employees through both prevention as well as safety issues/workers’ compensation. Wellness programs and rewarding for engaging in healthy activities can shave quite a bit off of healthcare spending.- As mentioned, the transition to value-based healthcare is not an overnight venture. One of the most difficult issues to circumvent is the need for a culture change. Time and energy should be exerted to change the culture from the top down. Empowering employees to be able to make changes to increase quality and decrease costs is monumental. Instilling buy-in from all levels of the organization is critical. Learning all of the processes from the front line rather than from senior management will assist in bridging the gap from fee for service to value based.
Defining Value is Difficult.
Value is really from the patient’s perspective. It is costs versus benefits. What do I have to give up and what will I receive? Costs aren’t just monetary but can be intrinsic as well such as customer service. Strides are being made daily towards value and quality. Organizations and practices should begin moving in this direction as quickly as possible. For now balancing fee for service as well as many other payment models is a challenge.
BHM Healthcare Solutions
If you need assistance transitioning to new healthcare reform payment options or assistance in trying to eliminate wastes and enhance efficiencies, please contact BHM Healthcare Solutions 1-888-831-1171 or re*****@*******pc.com. Our Healthcare Transformation Solutions can assist you in attaining and exceeding your goals.
