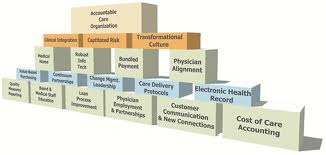
Summary: Accountable Care Organizations (ACOs) are gaining in popularity as a result of the Affordable Care Act. Have you considered the benefits of ACOs from both the patient and provider perspectives?
One of the goals of the Affordable Care Act (ACA) is to provide coordinated care which, in turn, increases quality and efficiency within the healthcare field, and reduces costs.
ACOs – What is an ACO?
ACOs are groups of providers which form an organization based upon the Medical Home (or PCMH) concept. The Medical Home places responsibility for the coordination of care with the primary physician. The primary care physician coordinates with other physicians and providers such as specialty physicians, laboratories and diagnostic imaging, providing a central point for the patient’s medical information. Additionally, patients are involved in the discussion surrounding their care, promoting a two-way dialogue as opposed to the traditional one-way. Patients have input rather being told their course of treatment. Building upon the Medical Home concept, ACOs are groups of Medical Homes working together to provide a more efficient health system, enhancing patient outcomes.
ACOs- Benefits to Patients
ACOs provide many potential benefits to patients.
- Accessibility – ACOs and Medical Homes are focused upon increasing accessibility for patients. Under these models, the typical 9-5 banker’s hours are no longer an option. Providers are extending hours to evenings and weekends. Same day, or on the outset, next day appointments are made possible. Medical records can easily be accessed by providers involved with the patient’s care. Population management is beginning to take hold to provide better, diagnosis, treating and tracking.
- Care Coordination and communication – The concept of ACOs is to provide a care team which coordinates efforts to provide better patient care. Communication lines are open among providers as well as between primary care and patients. If a patient needs to find out about a test that was run by a specialist, he can easily contact his primary care physician and obtain this information. Information is right at the primary care physician’s finger tips.
- Better Quality Care at a Lower Cost – ACOs are focused upon providing quality outcomes while simultaneously reducing costs. Under ACOs, only necessary tests are run. Reimbursement is based upon quality as opposed to quantity. Additionally, with the emphasis on care coordination, providers can easily check to see what tests/services have previously been performed. This avoids duplication and makes strides toward reducing costs for both unnecessary and duplicate tests/services.
- Reduced Paperwork – An ACO also benefits patients by reducing the amount of paperwork required to be completed. All of the medical records are right there and readily accessible. The emphasis becomes more on verifying pertinent information such as insurance and census data rather than spending hours filling out paperwork and filling out the same paperwork for different providers.
- Primary Care Physician – Under a Medical Home and ACO model, the primary care physician serves as the primary contact for all medical questions, issues, or requests for medical information. The primary care physician is responsible for coordinating care and obtaining all relevant medical information from other providers including specialists, laboratories, and diagnostic imaging. It becomes as easy as one-stop shopping.
- Two-Way Communication – ACOs provide a means of two-way communication with their primary care physician. Patients become involved in the decisions surrounding their healthcare. No longer does the physician just determine treatment without patient input, but it becomes a give and take conversation. Discussions around the different options available take place with the pros and cons of each, whereby the patient and the provider jointly make the decisions as to the best course of treatment.
ACOs – Benefits to Providers
ACOs are beneficial not only to patients, but also to providers.
- Stepping Stone to Pay-for-Value – As mentioned above, healthcare as we know it is transforming from fee-for-service to fee-for-value. Reimbursement models are emerging which reward for quality and value as opposed to quantity and volume. Some of these new models include bundled payments, value-based purchasing, and Accountable Care Organizations. As part of the transition to a true-value based delivery system, ACOs provide a stepping stone in this process. Processes and protocols begin to be established. Infrastructures begin to take shape. EHR and other information technology systems begin to transform. Mindsets begin to shift. Profitability begins to be realized.
- Patient Retention – Not only are providers transitioning to an emphasis on value, but patients are becoming more savvy as well. The bar has been raised and will continue to do so in terms of quality outcomes and patient satisfaction. Patient’s expectations are continuing to rise. When providers focus on quality, safety, satisfaction, and value, patients form loyalties with these providers. The providers become not providers of convenience, but providers of choice. When patients are happy, they create a ripple effect and positively recommend to their family and friends.
- Provider Profitability – Provider profitability is realized through successful ACO efforts and based upon coordinated care which provides efficiencies, quality outcomes, and reduces healthcare costs. The amount of potential profitability is determined by the amount of risk undertaken.
BHM Healthcare Solutions – www.dev.dev.bhmpc.com
Do you need assistance with transforming to an ACO? Do you need assistance with implementing new delivery systems such as bundled payments? BHM is a healthcare management consulting firm, with one of our many specialties being provider or physician compensation. For more information on these services, please view our Accountable Care Organization Conversion page or our Financial Analysis page.
Contact us to see how we can best assist you with your healthcare consulting needs. 1-888-831-1171 or re*****@*******pc.com.
