A burnout is defined as a “loss of enthusiasm for work, feelings of cynicism, and a low sense of personal accomplishment.” No profession is safe from workplace stress– but did you know that medical professionals are more likely than people in other professions to experience a burnout? From nurses to doctors, healthcare providers are feeling the affects of healthcare reform just as much as system administrators. Here’s what you need to you know about not only the physician burnout, but a medical professional burnout in general.
1. The Physician Burnout Is Real
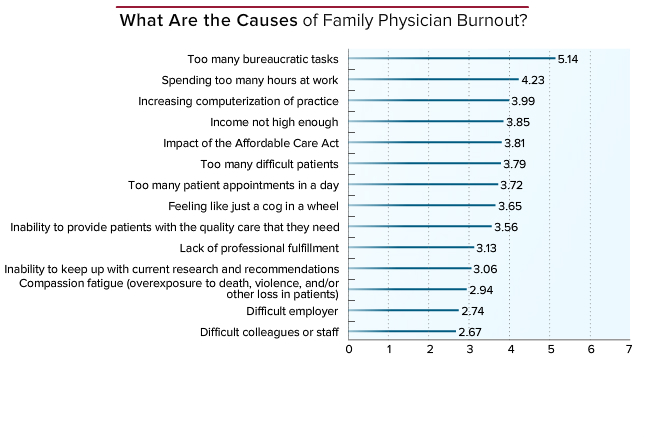
According to a Medscape survey, it’s reported that 30 to 40% of doctors experience some sort of emotion, physical or psychological stress in relation to their jobs. What’s causing it? Most medical related burnouts stem from long work hours, demanding on-call duties, and difficulty with the work/life balance. In addition to demanding schedules it’s also believed that many healthcare reform aspects, such as increased electronic record keeping or patient centered care, are big stressors for medical professionals. Who is being hit the hardest? “Emergency care, critical care, and family medicine workers experience the highest rates of burnout among health care providers.” In a survey completed by the Physician Foundation in 2014 it was found that a staggering 81% of physicians describe themselves as “overextended or at full capacity.” This number has increased dramatically since 2012, which found only 75% of doctors feeling overextended.
2. The Burnout Isn’t Just Doctors
Doctors are often the main subject in the discussion on healthcare burnouts, but nurses and other medical professional also are experiencing an increase in workplace stress. Nurses are among the many medical professional facing workplace burnouts. The Huffington Post reported “nursing remains one of the fastest growing workforces in the U.S., there is still a great shortage longing to be filled. As a result “researchers and nurses alike have already identified under-staffing as a leading cause of burnouts.” In addition to under-staffing “lack of social support, inability to control one’s work schedule or assignments, a chaotic or monotonous job and work-life imbalance” are also contributing factor to the nurse/medical professional burnout. From nurses to support staff to doctors, it’s clear medical professionals are all clearly suffering from of workplace stress. Keeping the burnout term broad (including nurses and other support staff) will be key to fueling a healthy discussion on the issue.
3. After Effects
Patient care, medical errors and miscommunication are just among the many side effects of the medical professional burnout. This is why is paying attention to the physician burnout so crucial. An blog post by The Joint Commission reported that “Increasing amounts of stress can negatively affect thoughts and attitudes, while building frustration, anger and resentment. In more extreme cases this can lead to impaired judgment, communication gaps or performance liabilities. All of these can affect the patient-physician relationship or the treatment the patient receives.”

4. How To Recoup
What can we do? Mindfulness is one of the most common ways healthcare systems are dealing with burnouts. Medscape describes mindfulness as “mental training that enables one to attend to aspects of experience in a nonjudgmental, nonreactive way, which in turn helps cultivate clear thinking, equanimity, compassion, and open-heartedness.” One Hawaiian hospital has implemented a strategy called, “Code Lavender.” This special program “aims to support nurses and physicians during emotionally troubling or exhausting times, often after experiencing the death of one or several patients.” From meditation to message, it’s a new approach but researchers are finding that focus is actually helping to reduce stress and improve the well-being of medical professionals.
In an article for WIRED Dr. Linda Girgis suggests that in its own way, social media is helping to reduce physician burnout by helping medical professional find their voice. Girgis reports that social media is great tool physician collaboration and in the long run may “have the indirect benefit of mitigating the stress and anxiety of running a medical practice.”
5. The Future
Medical professionals are the core of patient care and their well being not only effects the patient who they interact with but the overall quality of a healthcare system. More often than not medical professional burnout is seen as inevitable side effect of the trade and not treated an issue for a healthcare system at large. Changing the way we think of stress, educating and preparing all staff will be a key tool in moving forward. Providing awareness and support for burnout symptoms, joining forces for the cause, will benefit everyone in the long run. It should be made clear that it’s not all bad news. In a 2014 survey by the Physician Foundation found that “44% of physicians describe their morale and their feelings about the current state of the medical profession as positive, an increase from 32% in 2012.” Combining this positive view of the medical profession with the new approaches to medical professional burnouts just might be the secret to getting ahead of the epidemic.

