| BHM integrates behavioral health through our independent review services. Our network compliments your organization’s push for integration with over 500 practicing clinicians. Click here about how this approach and expertise sets BHM review services apart. |
Primary care providers are no strangers to Behavioral Health Integration. Many individuals with behavioral health conditions pass through primary care settings daily. One in five Americans suffer from behavioral health conditions, leading to an estimated $57 billion per year in costs (1). Mental health issues are frequently unrecognized and often reimbursement for behavioral health services is not an option. This has resulted in primary care providers and payers integrating behavioral health services into model of care.
The Treatment Gap
- Patients- Symptoms of mental illness may reduce a patient’s ability to initiate and follow through with treatment.
- Primary Care Providers- providers may feel uncomfortable treating patients with mental illness.
- BH Providers- May lack knowledge or expertise to provide medical care for their patients
- Payers- Payment models can be complex, making reimbursement for behavioral health services difficult
- System Gap- Fragmentation between BH and PC can result in patients receiving inadequate or uncoordinated care
Integration Models for Primary Care and Behavioral Health Integration
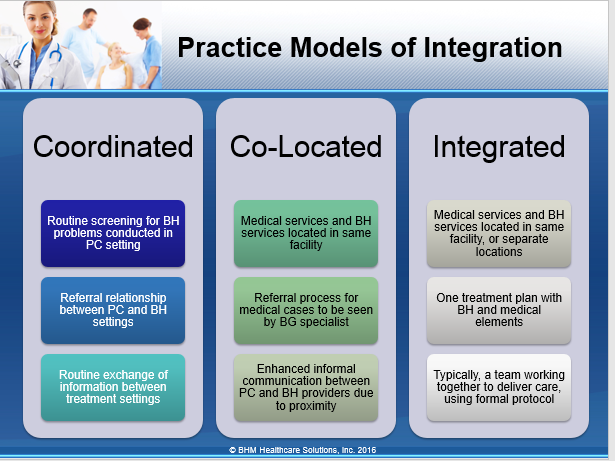
Integration Tips for Payers
- Change payment models to include reimbursement for behavioral health services
- Embrace value-based payment models (accountable care, value based payments)
- Collaborate with primary providers and behavioral health professional to create standardized measures for BH integration best practices and quality outcomes
- Activate billing code sets for care and case management services. This way services integrated settings can be properly documented (2)
- Include behavioral health claims in your Peer Review Program
- Think about reimbursing for telehealth services
BHM integrates behavioral health through our independent review services. Our network compliments your organization’s push for integration with over 500 practicing clinicians. Click here about how this approach and expertise sets BHM review services apart.
