
Industry Watch Alert
The March 31, 2026 deadline marks the first public reporting milestone for prior authorization metrics under CMS-0057-F.
Impacted payers are now required to place plan-level prior authorization performance data on their websites, opening a new chapter in utilization management transparency.
As reporting becomes public, prior authorization operations move further into view as a measurable signal of administrative performance and process discipline.
CMS requires impacted payers to publicly report 2025 prior authorization metrics by March 31, 2026, creating new transparency around denial rates, appeals, and turnaround times.
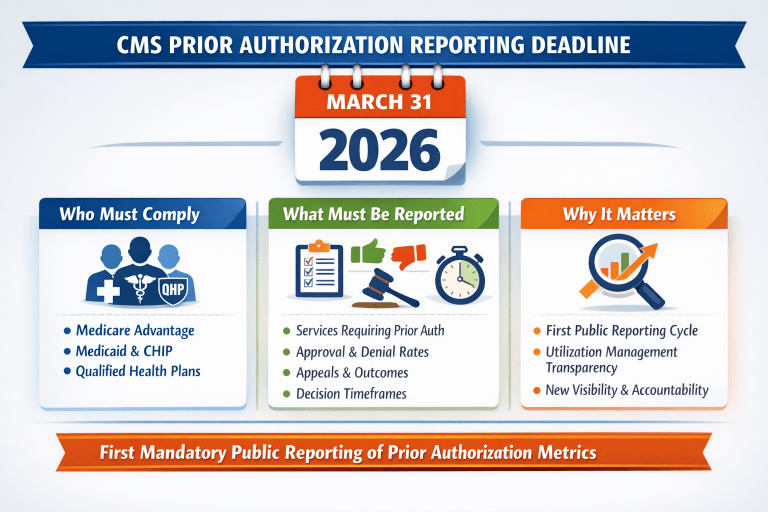
March 31, 2026 is the first deadline for impacted payers to publicly post prior authorization metrics for the previous calendar year under CMS-0057-F.
The requirement applies to Medicare Advantage organizations, Medicaid managed care plans, CHIP managed care entities, and Qualified Health Plan issuers on the Federally Facilitated Exchanges.
Public disclosures must include key prior authorization performance data such as the list of items and services subject to prior authorization, approval and denial rates, appeal outcomes, and average decision timeframes.
This marks the first mandatory public reporting cycle for prior authorization performance data, creating a new level of visibility into utilization management operations.
Executive Summary
A major prior authorization transparency deadline is now here for impacted health plans. Under CMS’s Interoperability and Prior Authorization Final Rule, impacted payers must publicly report certain prior authorization metrics for calendar year 2025 on their public-facing websites by March 31, 2026.
This reporting requirement is not limited to broad policy language. CMS has outlined a specific reporting structure that includes public disclosure of the items and services requiring prior authorization, prior authorization request volumes, approval and denial rates, appeal data, and average decision turnaround times. CMS also published a reporting overview and template to support payer compliance.
The significance goes beyond compliance. For the first time, providers, beneficiaries, and other stakeholders will have direct visibility into plan-level prior authorization performance data. That shift may increase scrutiny around operational efficiency, consistency of determinations, denial trends, appeal outcomes, and overall responsiveness in utilization management processes. CMS has framed these policies as part of a broader push to improve transparency, reduce burden, and hold organizations accountable for prior authorization practices.
For payer organizations, the practical issue is not just whether the data is posted on time. It is whether the underlying workflows, documentation standards, review practices, and decision timelines can withstand public and regulatory visibility. Plans that are still treating this as a website posting exercise may be missing the broader operational and reputational implications.
Public reporting of prior authorization metrics changes the conversation. Beyond compliance, it creates a visible record of how prior authorization programs function in practice, including turnaround times, denial activity, and appeal outcomes.
As payer organizations adapt to this level of transparency, consistent clinical review processes, defensible documentation, and disciplined utilization management oversight become even more important. BHM Healthcare Solutions supports payer organizations with independent clinical review, utilization management expertise, and quality oversight to help prior authorization programs remain consistent, defensible, and aligned with evolving regulatory expectations.
Previous Alerts
Sources
Centers for Medicare & Medicaid Services (CMS)
CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F)
Centers for Medicare & Medicaid Services (CMS)
CMS Interoperability and Prior Authorization Final Rule Fact Sheet.
Centers for Medicare & Medicaid Services (CMS)
Prior Authorization Metrics Reporting – Overview & Template.
Centers for Medicare & Medicaid Services (CMS)
Prior Authorization API Frequently Asked Questions.
Centers for Medicare & Medicaid Services (CMS)
CMS-0057-F Final Rule PDF.
FAQs
What is the CMS prior authorization public reporting deadline?
Impacted payers must publicly post prior authorization metrics for the previous calendar year by March 31 each year, beginning with 2025 data posted by March 31, 2026.
Which payers are subject to the reporting requirement?
The requirement applies to Medicare Advantage organizations, Medicaid managed care plans, CHIP managed care entities, and Qualified Health Plan issuers on the Federally Facilitated Exchanges.
What prior authorization metrics must be reported publicly?
CMS requires public reporting that includes the items and services subject to prior authorization, certain approval and denial data, appeal outcomes, and average decision timeframes for prior authorization requests.
Each week, we email a summary along with links to our newest articles and resources. From time to time, we also send urgent news updates with important, time-sensitive details.
Please fill out the form to subscribe.
Note: We do not share our email subscriber information and you can unsubscribe at any time.
|
|
Thank you for Signing Up |

Partner with BHM Healthcare Solutions
BHM Healthcare Solutions offers expert consulting services to guide your organization through price transparency & other regulatory complexities for optimal operational efficiency. We leverage over 20 years of experience helping payers navigate evolving prior authorization requirements with efficiency, accuracy, and transparency.
Our proven processes reduce administrative errors, accelerate turnaround times, and strengthen provider relationships, while advanced reporting and analytics support compliance readiness and audit preparation. From operational improvements to strategic positioning, we partner with organizations to turn regulatory change into an opportunity for clinical and business excellence.
