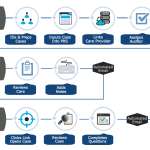
Intelligent Document Processing for Payer Cost Savings
Intelligent Document Processing (IDP) is a technology that uses artificial intelligence (AI) and machine learning to automatically extract and process data from documents such as claims forms, invoices, and medical records. This eliminates the need for manual data entry and speeds up the processing of claims and other documents.