The Triple Aim, Explained.
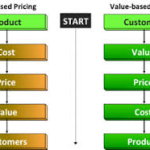
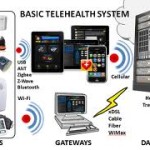
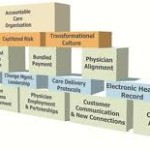
With hospitals moving toward a value-based payment system there is more demand now than ever for strategies that will help healthcare systems hone in on population health. The Triple Aim, an initiative set forth by the Institute for Healthcare Improvement, covers three main checkpoints for all hospitals as they make this transition.