Payers are stretched to the breaking point trying to manage the onslaught of substance use disorder cases. It’s more important than ever to acquire accurate data to help payers and policy makers establish effective and long-lasting opioid crisis measures.
In a report from the New England Journal of Medicine, these opioid prescription control policies are closely examined. The effectiveness of the programs assist policy-makers on their mission to combat the opioid crisis. The paper argues that there are two theories central to opioid prescription control policies:
- Reducing prescriptions will also reduce the quantity of drugs available for abuse
- Reducing prescriptions will reduce the chances of option use disorder for first time opioid users
The examination focused on data collected from reducing opioid prescriptions in Massachusetts, the state with the seventh highest rate of opioid overdose deaths in the United States in 2015.
The collection of policies include: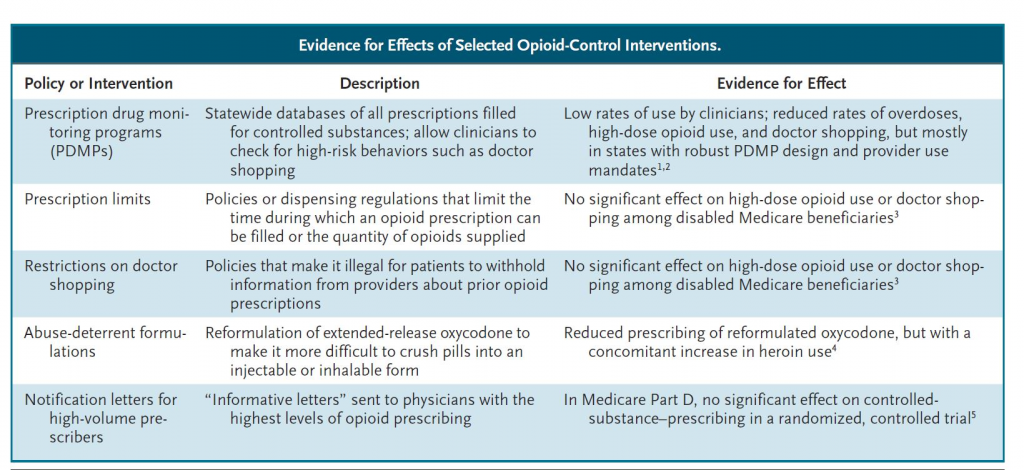
These prescription-opioid-control policies are having mixed effects. A major challenge in examining a rapidly evolving crisis is that there is little time to waste on ineffective or counter- productive policies. Resources are sparse and the crisis is at its peak.
Productive collaborations among policymakers, data collectors, and government officials could help identify lifesaving policies worth spreading.
For payers and policy-makers it can be a challenge to design effective opioid crisis measures to control the rapid increase of overdoses as program effectiveness data is being accumulated. Staying abreast as to how opioid prescription control policies are evaluated for effectiveness, payers can be more efficient in their policymaking. Click HERE and discuss how BHM helps track claims data for payers.