 Key Elements of an Optimized Healthcare Revenue Cycle
Key Elements of an Optimized Healthcare Revenue Cycle
Revenue is the very lifeblood of hospitals and other healthcare providers. And clearly, the more effective your revenue cycle management processes are, the more certain you can be of continuing to fulfill the mission of healing.
The Building Blocks of Healthcare Revenue Cycle Improvement
As defined by the Healthcare Financial Management Association (HFMA), revenue cycle management encompasses “all administrative and clinical functions that contribute to the capture, management, and collection of patient service revenue.”
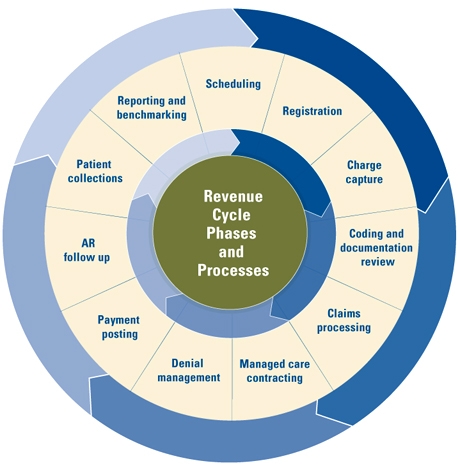
To optimize your healthcare revenue cycle management processes, it pays to critically evaluate the following components:
Pre-registration – it all begins here, before the patient even arrives for treatment. Patient registration information – including eligibility, benefits, and authorizations – can be collected via phone, or as is increasingly prevalent, online, via a patient portal. This is the first step in the revenue cycle, and therefore, your first chance to get it right – or wrong. Errors made at this phase inevitably complicate, and potentially, compromise the entire revenue cycle process.
Registration – like pre-registration, the actual registration process is crucial to effective revenue cycle management. The patient information you collect here is essential to satisfying clinical, financial, and regulatory requirements. This is also your first opportunity to begin collecting revenue, in the form of co-pays, deductibles, and outstanding balances. Many practices have begun to implement a policy of offering bonuses to staff members who most effectively collect these types of payments at the time of registration. Remember, funds you collect now are funds you will not have to pursue at a later date – which can be a costly and time-consuming process.
Coding and charge capture – perhaps among the most complicated phases of the revenue cycle, coding and charge capture are also among the most critical. Here, documented services are translated into billable fees via the use of a complex set of universal medical code numbers, which describe diagnoses and procedures performed. Properly coding the services you provide can make an immense difference in the actual revenue you generate. If you haven’t already done so, consider ongoing training for your coding staff. Additionally, coding standards change rapidly and with great regularity, therefore the importance of maintaining proficiency in this discipline cannot be overestimated.
Claims submission – this is the point at which billable fees are submitted to payers. In addition to actually receiving payment, the other primary objective at this phase is to minimize the potential for claim rejections and subsequent resubmissions. You’ll also want to make every possible effort to expedite payer responses to the claims you submit. Among the many common errors that can derail your claims submissions are missing or incomplete codes, invalid or missing authorizations or referral numbers, incomplete form fields, and even handwritten claims, which are no longer accepted.
Denial Management – industry studies indicate that approximately 25-30% of healthcare claims are rejected or denied, resulting in tremendous losses to healthcare providers. The majority of these losses can be avoided by implementing an effective denial management process. All effective denial management strategies involve the following two initiatives:
- Denial assessment – dynamic data gathering and analysis to pinpoint denial causation by type and payer.
- Implementation – processes to reduce or eliminate denials.
Patient collections – this is the process of collecting payments from patients for services rendered. One important trend in this area is the adoption of electronic payment systems using online patient portals.
Some General Healthcare Revenue Cycle Tips:
- Know your data – the better you understand your payment trends, the better equipped you’ll be to recognize where and how you can improve your revenue cycle processes. You may wish to consider implementing an enterprise data warehouse (EDW), which lets you combine and analyze clinical and financial data in ways that can help you gain real and measurable advantages.
- Set goals – understand the data you collect and, using this data as a baseline, set measurable performance goals. Monitor progress as you go, and consider establishing pay-for-performance initiatives where appropriate.
- Monitor payer contracts – are your payers reimbursing you at the levels you expect? Are they consistently denying more claims than you believe they should? Be aware of the trends and be prepared to communicate openly with your payers in the event that need to do so.
The Direct Route to Optimized Healthcare Revenue Cycle Management
Effectively managing the revenue cycle can be a daunting task. Fortunately, BHM offers the expertise you need to achieve the success you desire. Using our revenue cycle management strategies, BHM clients have experienced improvements in cash flow of up to 22%. Contact us today to find out how BHM’s proven strategies can work for you.
Email: re*****@*******pc.com
Phone: 1-888-831-1171
