NCQA Health Plan Accreditation: 5 Reasons for Third-Party Review
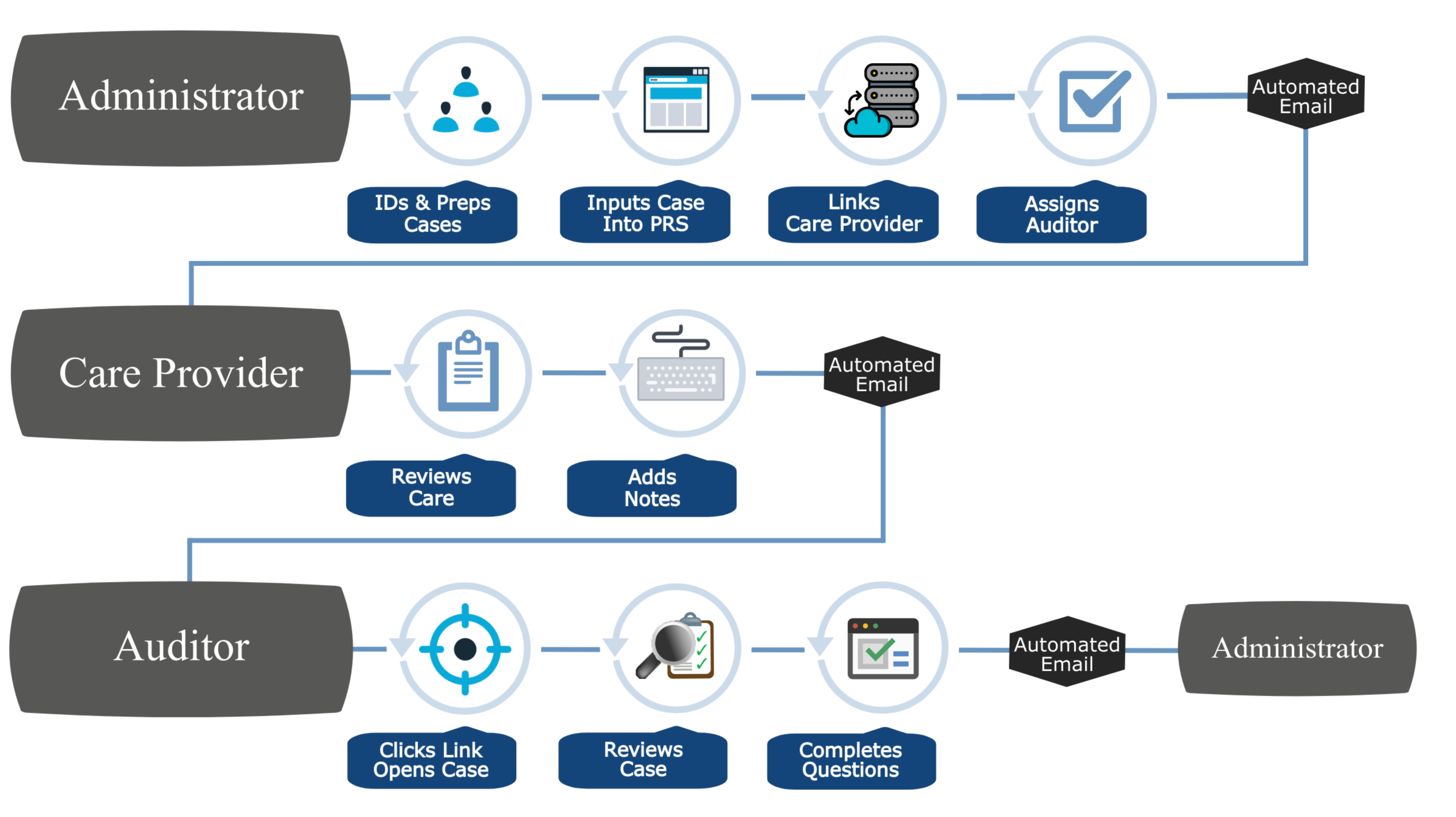
NCQA Health Plan Accreditation is a rigorous evaluation process that assesses the quality of health plans and their ability to meet the needs of their members. As part of the accreditation process, NCQA requires health plans to undergo third-party review.